Abstract
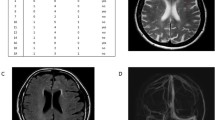
Anderson-Fabry disease (AFD) is an X-linked recessive lysosomal disease caused by alpha-galactosidase A (alpha-gal) deficiency, causing progressive glycosphingolipid storage in various organ systems. Headache is a frequent symptom. Cerebral magnetic resonance imaging (MRI) often shows multiple white matter lesions (WML), like those seen in patients affected by migraine, in particular with aura (MA). To our knowledge, there are no reports about the prevalence of AFD in patients with MA. The objective of the study was to determine AFD prevalence, as assessed by alpha-gal activity and genetic tests, in MA patients. We evaluated 73 consecutive patients followed by the Headache Centre of our Department with a diagnosis of MA. They were screened for migraine characteristics and cerebrovascular risk factors. Gaseous contrast transcranial Doppler was used to diagnose right-to-left shunt and MRI to detect WML. All patients underwent blood test to evaluate peripheral alpha-gal activity and to identify alpha-gal gene mutations. Of 73 consecutive screened subjects (59 females, 14 males; mean age 38.3 ± 11.8 years), the known GLA pathologic mutation p.[Asp313Tyr] was found in a 38-year-old woman, with a history of MA, deep venous thrombosis and abdominal pain. Cerebral MRI showed small WML. This is the first study reporting AFD prevalence in a cohort of MA patients. We found a relatively high prevalence (about 1.37%) among the examined patients, even if this finding needs to be confirmed in a larger sample. Despite this high prevalence, it seems not necessary to screen systematically all MA patients for AFD, but since it is a treatable genetic disorder, it is worthwhile to consider it for the subgroup of patients presenting WML and other typical AFD symptoms.
Similar content being viewed by others
References
Fellgiebel A et al (2006) CNS manifestations of Fabry’s disease. Lancet Neurol 5:791–795
Ries M et al (2003) The early clinical phenotype of Fabry disease: a study on 35 European children and adolescents. Eur J Pediatr 162(11):767–772
Sims K et al (2009) Stroke in Fabry disease frequently occurs before diagnosis and in the absence of other clinical events. Stroke 40:788–794
Mehta A et al (2004) Fabry disease defined: baseline clinical manifestations of 366 patients in the Fabry Outcome Survey. Eur J Clin Invest 34(3):236–242
Rolfs A et al (2005) Prevalence of Fabry disease in patients with cryptogenic stroke: a prospective study. Lancet 366(9499):1794–1796
Gibas AL et al (2006) A survey of the pain experienced by males and females with Fabry disease. Pain Res Manage 11(3):185–192
Swartz RH et al (2004) Migraine is associated with magnetic resonance imaging white matter abnormalities: a meta-analysis. Arch Neurol 61:1366–1368
Etminan M et al (2005) Risk of ischaemic stroke in people with migraine: systematic review and meta-analysis of observational studies. BMJ 330(7482):63
Headache Classification Subcommittee of the International Headache Society (2004) The international classification of headache disorders, 2nd edn. Cephalalgia 24(Suppl 1):9–160
Moore DF et al (2002) Elevated cerebral blood flow velocities in Fabry disease with reversal after enzyme replacement. Stroke 33:525–531
Moore DF et al (2002) Enzyme replacement reverses abnormal cerebrovascular responses in Fabry disease. BMC Neurol 2:4
Conflict of interest statement
The authors declare that they have no conflict of interest related to the publication of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Albano, B., Dinia, L., Del Sette, M. et al. Fabry disease in patients with migraine with aura. Neurol Sci 31 (Suppl 1), 167–169 (2010). https://doi.org/10.1007/s10072-010-0314-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-010-0314-5